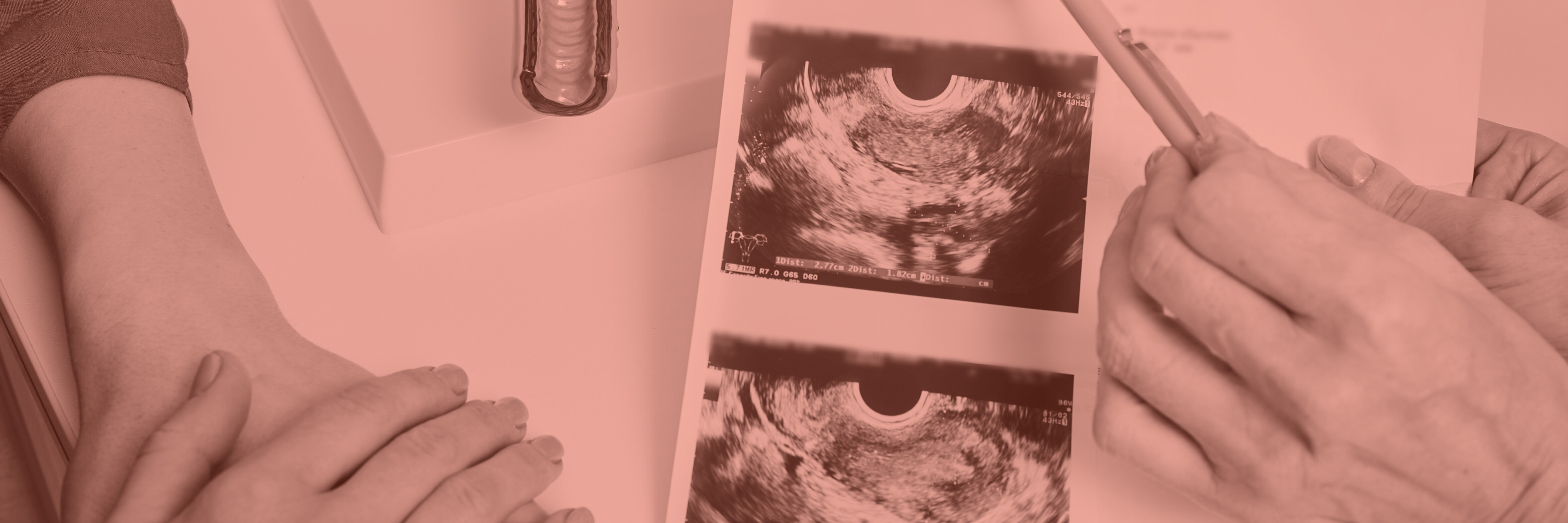
Caesarean Scar Niche Repair
A caesarean scar niche (also called an isthmocele) is a fluid-filled or pouch-like defect in the uterine lining at the site of a previous caesarean section scar. Many niches cause no symptoms and do not need treatment. When symptoms occur, surgical repair can be an effective option.
When might repair be considered?
Symptoms that may be linked to a niche include:
- Post-menstrual spotting or brown discharge for several days after a period
- Prolonged or irregular uterine bleeding
- Pelvic pain or dyspareunia (pain with intercourse)
- Subfertility or difficulty conceiving, when other causes have been considered
Diagnosis is usually made with transvaginal ultrasound; sometimes saline infusion sonography (SIS) or MRI helps define the defect. I will interpret imaging in the context of your symptoms and discuss whether surgery is likely to help, or whether other treatments are more appropriate.
Surgical approaches
There is no single operation that suits everyone. Depending on the depth and width of the niche, the thickness of the uterine muscle below the scar, and your fertility plans, options may include:
- Hysteroscopic niche resection — the niche is opened and trimmed from inside the uterine cavity, without abdominal incisions. Often used when the residual myometrium is thick enough to do this safely.
- Laparoscopic (or robotic-assisted) repair — the scar is exposed from the abdomen and the defect is repaired in layers, sometimes with removal of thin scar tissue. This may be preferred when the wall of the uterus at the scar is very thin or when hysteroscopic treatment is not advised.
- Combined hysteroscopic and laparoscopic steps in selected cases.
If you are planning future pregnancies, the choice of technique and timing of conception after repair are important — we discuss uterine rupture risk and delivery planning (often caesarean section) based on current evidence and your individual anatomy.
Recovery
Recovery depends on the procedure:
- After hysteroscopic repair, many people return to usual activities within a few days, with light bleeding or discharge for a short time.
- After laparoscopic repair, expect 1–2 weeks for light activities and 4–6 weeks before strenuous exercise, similar to other laparoscopic gynaecological surgery.
Read more in my Surgical Recovery Toolkit.

Dr Sam Holford
After a caesarean section
If your periods changed after a C-section, or you have persistent spotting or pain, a scar niche might be part of the picture — but not always. I can help you make sense of imaging and whether repair is right for you.
Book an appointmentFAQs
Please note: This information is general in nature and not a substitute for medical advice tailored to your specific situation.